Warning – this is my longest post yet, but I think it will serve well as something to revisit when I get the call and for months after. I will probably make a To-Do/Do Not Do list later.
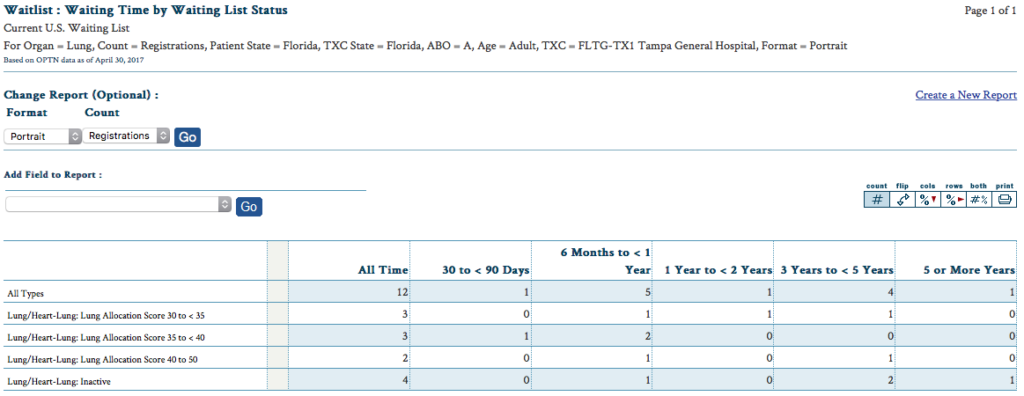
We’ve got some indicators that the wait may not be too much longer. There was another transplant performed with one of the 9 active people with my blood type at Tampa General, so now there are only 8 people to compete with. You can see from the report below that only 2 absolutely have a higher score than I have at 38.859, but I don’t know where the 3 of us in the 35-40 range fall against my score. I’ve emailed one of the coordinators to see if my name printed out for this transplant or any others that didn’t happen since my clinic visit. I’ll update this post and our Facebook group with the reply if it comes after I publish this.
What happens to the patient after transplant?
The stories vary a bit here, but the general timeline stands if there are no complications. This is a combination of what we’ve been told about our center and what I’ve learned from following CF transplants for a decade.
Surgery lasts 6-12 hours and they come out or call to update every couple of hours like, “The left lung is in now and it is a perfect match and fit. They’ve started the right lung.” The large variation in time depends on how difficult it is to remove the diseased lungs and how good of a fit the new lungs are. I’ve read on numerous CF blogs and in the transplant groups that CF lungs sometimes attempt to grow into the chest wall in a desperate attempt to survive. In those cases, the lungs aren’t simply disconnected and pulled out, but scraped out.
After surgery, patients are sent to cardio-thoracic intensive care (CTICU) for several days for very close 24/7 monitoring. One guy in support group said “Your job in CTICU is to give the nurses information about your status any time of day they ask, it’s not for rest or sleeping.” Once I’m in there, the primary support person is able to see the patient through their room window and are then told to go home and rest for 24 hours when they’re allowed to return and be in the room.
— I’m going to switch persons here to make the audience other patients because it’s about to get weird in this person (which also reads weird, too). —
You are secured by your wrists with restraints so you do not pull out the ventilator tube (being intubated), which is the natural reflex to do. The nurses are there when you wake up. They make sure you’re okay and stabilized as they wean you off the ventilator. At some point they pull out the tube that is all the way down your trachea and have you cough to get out any fluid that built up. “First breath” stories vary from being underwhelming to a mountain-top experience.
At some point before or after that, I’m not clear which, they sedate you again for a while. Within the first 24 hours, they have you sitting up in a chair. This is to let the lungs hang down and expand to fill the chest cavity. As someone with CF who has had his lung function slowly decline over 25 years to where it is now, I no longer take anything near a normal person’s deep breath. My normal breathing is a pitiful thing for someone with healthy lungs. The big challenge with new lungs will be to learn to take a deep breath worthy of the gift that’s just been received. Sitting up helps that. They also have bedside breathing devices that measure inhalation instead of exhalation. Right now I’m lucky to get 2L in a deep breath. Remember that figure – it will be wildly different post-transplant.
After surgery, they have two types of drain tubes placed in the chest cavity to prevent fluid build-up that would impinge the new lungs. They place between 4 and 6 larger tubes and a couple of thin tubes. They are uncomfortable, to say the least, but they are pretty quick to give an epidural for pain. No one I have spoken to at Tampa General has said they were in pain after surgery, which is an incredible relief to hear since lung transplants are the most difficult and dangerous of all solid organ transplants.
Between 18 and 48 hours after surgery (the next day seems to be what I see most often), the nurses stand you up and gather all the drainage tubes and devices, IV poles and tubes, and take you for a walk around the unit. It’s slow and steady (or unsteady) to start because of how much is hanging out of you,
As the days progress, they will remove more and more tubes and you walk further and further – miles, even. Things start to feel more comfortable and getting around gets much easier. All the while, they continue to draw blood every few hours to get your levels on the meds and adjust accordingly. They do everything for you. Now that I have a G-J Tube, I can get feeds without eating, but after a while, they perform a swallow test to approve you to eat by mouth. One recent person chose Mt. Dew and a candy bar. I’m right there on the drink idea.
As you gain in strength and adjust to being on so many new meds, they teach you and your support person about the medication routine, telling you each time what each one is for and when you’re taking it. In the past, for my entire life, medication has been the biggest issue in the hospital, so to see how it’s meant to be done by the best of the best will be much appreciated. I will finally let my guard down and trust the staff to not do something horrible.
What’s the deal with the new medications?
Any new organ is seen as a foreign invader to the body’s immune system, which says, “You are not like the rest of me, so I will eradicate you.” This eradication is called “rejection.” Organ rejection can take a couple of days or months, depending on why there is rejection and how acute it is under the supervision and medication. “A few missed doses of immunosuppressant meds and you’re toast,” is what I was told. This is one reason why CFers are so successful with transplants compared to people who smoked and got COPD or someone who got some acute pulmonary illness that took them from healthy to dying. We are used to taking meds every day. We’re also typically 1/2 to 1/3 the age of most of the other diagnoses when transplanted. The people in support group could all be my grandparents, so I’ll naturally bounce back from surgery faster than them just based on age.
Immunosuppressants will take my immune system all the way down, just shy of chemo state. In fact, chemo is used when nothing else is helping solve a bad case of rejection. They simply nuke the immune system away until the attack stops. This means I will live in a bubble for a little while. I’ll wear a mask any time I go outside for 2-3 months and for several months after that when I go inside with other people, like the stores or church.
Also some foods are off the list after transplant are undercooked meats, so no sushi or steak less than well done. Yes, I am a rare steak eater, and that will be my biggest sacrifice post-transplant. Buuuut… breathing… rare steak… living… rare steak. Ok, well done steak, it is!
They also discourage gardening, buffets, and doing much of anything where water, mold, and dirt are involved together. There are many fungi in situations like mowing, garden dirt, or pressure washing. I currently have a fungus in my lungs that prevents me from staying on Prednisone to feel better because the fungus would thrive in that environment and take me down instead of feeling better on steroids. Some foods interact with the meds, like grapefruit – I hate grapefruit anyway.
However, most precautions revolve around infection potential and these warnings vary from center to center and you also have to decide if you’re going to live in a bubble or go enjoy life. It’s an incredible balancing act.
I should be cutting out most, if not all of my inhaled meds and chest physiotherapy that makes me get up 2 hours before everyone’s day starts. Some people and some centers keep people on some inhaled antibiotics for a few weeks or months, but rarely longer than that, but since you can catch something so easily, the need might arise to take antibiotics at any point.
One of the big dangers post-transplant is cancer, due to the immune system. Skin cancer is all the rage with Florida patients and our newfound love and ability to go out and enjoy life. I’ve long been living a shady life – a solid decade at least. My golf tan from my HS golf team days has long been gone. We’ve stayed under the trees and a canopy our entire time dating and in marriage. I stay under the cover at the neighborhood pool. I’ll start wearing long-sleeve shirts and hats even more than I do now.
With the nasty, infected lungs gone, your body no longer needs to fight against such a raging infection 24/7/365, so we start to put on weight in a massive way. Between tube feedings and my food not being spent on infections, I fully expect to gain 10lbs per month for 3-6 months. At that point, we’ll be doing a fundraiser for new clothes. I kid, I kid! We love Goodwill and I have lots of clothes from my brother-in-law that are too big for my ideal weight.
What happens for family and friends after transplant?
It’s pretty common for everyone to want to come over and see the newly transformed friend or relative. As I said earlier, I’ll live in a bubble for a little while. Whenever anyone does come over, we have a sanitation station complete with a mask and glove box. When Boy comes home from school every day, he’ll go straight upstairs to change his clothes into “home clothes” and wash up.
I’m switching to first person now because this is what we’ll be doing, or what I/we plan at this point.
A quick note, things could go less than ideal before discharge. The number of complications are vast, but usually revolve around gastro issues or temporary issues with getting the lungs to settle/inflate/heal in the “normal” amount of time. One person was recently in for over a month and had and additional surgery that delayed leaving. Barring issues, I expect to be home within 14 days. There are also issues that carry with the new lungs. One of them is cytomegalovirus (CMV). It’s what causes mono in kids and often never shows symptoms, but is carried unseen. With a weak immune system, it can flare up, much like shingles do decades after getting chicken pox. These things will forever be a possibility and something that we chase down numerous times.
While I’d love visitors in the hospital, that’s probably very close to out. It’s definitely not ideal while in CTICU, but manageable in the step-down unit. I think I’d prefer to FaceTime and stick to this site and Facebook. I have my wife to update them and a close friend who has access to this site to publish and keep up with donations or sidebar items. Most of our friends have school-age kids or grandkids and could be carrying something without knowing it. I’d rather not take that chance in the hospital.
Instead, the sidebar has the mailing address for the hospital (don’t forget my name in the address). It’d really lift me up if that got flooded and we could put cards everywhere and I’ll be spending a lot of time in the chair and out walking when I’m discharged. I promise we will be taking lots of photos and videos. I might even brave a Facebook Live walk down the hall once we have some saved on our devices and can possibly schedule a walk to announce it beforehand. How cool would that be!?
While admitted, we will need the entire townhome and both cars completely sanitized from my past infectious germs. My mother-in-law is leading the charge there but the list includes:
- dusting and wiping all surfaces… possibly re-painting the walls (I don’t think we have a consensus on that because of how much stinking work that would be)
- sanitizing anything that I use – keyboards, pens, toiletries, glasses, drink bottles, etc.
- deep-clean the carpets and tile
- burn my car to the ground, collect $300 insurance
- clean/sanitize air ducts/vents
- sanitize or replace indoor air handler (currently very suspicious condition)
- UV light in the air handler
- replace all air filters, everywhere – vacuum cleaner, car cabin filters, A/C unit
- replace water filter in refrigerator
- I have a reverse osmosis filter kit that someone could look into installing in the kitchen
So you can see there is a lot for my support network to handle for me while my only job is to stay alive with improving excellence in breathing for a solid month. How do you like me making two jobs into one? That’s something only an English degree can buy.
After the point we get me back home, we don’t have a clear picture of what we will need and what we should accept with concerns about any dietary items or safety protocols we still don’t know about.
The biggest change apart from my ability to breathe will be my medication and morning routine. I’ll make no effort to work for the first 2-3 weeks after discharge, so I think my new routine will include a lot of deep breathing, walking around, exercises, and enjoy not being tethered to an oxygen hose.
The second biggest change will be that I will not be allowed to be left alone for 3 months. I can’t stay home while my wife does the school runs or errands. I think we’ll get lots of quality time together if she’s not tired of me after taking care of me for a week or two in the hospital or however bad I get before I get the call. 🙂 The morning drop-off is quick, but picking up takes about an hour. Everywhere I go in public, I’ll be wearing my 99% particle blocking mask.
I’m going to be quite eager to get out and see people in public places to catch up with friend and family and maybe dance a jig or do some jumping jacks. Some things will take coordination, like if my wife drives me to men’s group, I’ll need a lift home or if we are out doing an activity, someone will need to stay with me at all times, so I won’t be getting any introvert time on long days with people. Being an introvert was a bit of a built-in help when I was having a bad lung day because I’d sit and chill while everyone went around the kid’s area at Busch Gardens. Now I’ll be right there with them or we’ll be going with others. Minor things, really, but things to sort out.
Hey, alive beats dead!
After my meds stabilize, I’ll be cleared to drive again. Then drive alone when my wife feels comfortable. Around that time, we’ll probably start doing extended family stuff in homes.
The big rule after transplant is that if anyone has been around anyone who may be sick, they need to not come or I need to not go if it’s their house. It’s hard, because when people make plans to do something, it sucks to cancel because you have a runny nose or sore throat. What sucks more is a life-threatening infection. I’ll definitely wear a mask at church because no one stays home when they’re sick. I’m even guilty of that.
I think this is enough words – pushing 2500 now.