Right out of the gate… thank you to everyone who prayed, texted, liked, favorited, replied, shared, and visited us on our adventure after receiving The Call Friday morning. As eloquent as my words can be from time to time, they fall pitifully short of being able to describe how much love we felt from all over the globe.
I’m going to mostly stick to the narrative in this “essay,” as my geek friends are calling my posts, and expand on my heart and mind in another one quickly following this. This one will serve as a detailed (my longest post ever) personal experience for anyone following to know what the process is like, at least at Tampa General Hospital in 2017.
The link will go here → How I Felt on “Dry Run Day” and After
For those who don’t want all of the details or are busy, I wrote a TL;DR at the end.
June 9, 2017
Thursday night, my wife went to bed and I fully planned on watching an episode or two of Sherlock Holmes on Netflix before succumbing to sleep, but soon realized 5 minutes into my attempt that it was time to fully recline my chair and roll over. Every weekend has been busy, so I second-thought the wisdom of staying up late in case The Call came Friday, Saturday, or Sunday.
For the first time in 84 1/2 days, my guard was down.
The Call
2:16am – [phone rings]
I bolted half up in my chair towards the end table and pulled my phone to an inch from my eyes so I could see blindly without my glasses and saw “Clinic 24/7” was calling me… and it was only 2am. (!!!!) There was no mistaking what this was. No wrong number, no butt dial, no auto warranty spam call. THE CALL.
“Hello!” I said in my most chipper, “I’m up and alert” voice.
“Hello, is this Jesse Petersen?”
“Yes it is,” I said much less convincingly of my awake status.
In the calmest, most professional tone I’ve ever heard, the voice said, “I’m Shari from the Tampa General lung procurement and we would like to make a preliminary offer of some lungs to you.”
In my haze that was coming quickly back, I was thrown off by the word “preliminary” and asked if I was the backup recipient, to which she said I was not but that I was primary and she continued with her information. In my stupor, I started rooting around the end table and my pockets for my wallet to get out my pre-prepared “The Call paper” to take notes, but I was coming up null. Then I started an epic coughing spasm as always happens when I get up from sleep.
“I’m so sorry about that,” after I brought the phone back to my face.
“No problem at all. It sounds like we should get you some new lungs today, how about that?”
 She went on to tell me that the donor was considered high risk and she went on to read me required language about what triggers that label and tell me more. Meanwhile, I’d walked upstairs and opened the door to our bedroom and my wife bolted up and knew something was up. I put the call on speaker and she heard everything after the high risk triggers.
She went on to tell me that the donor was considered high risk and she went on to read me required language about what triggers that label and tell me more. Meanwhile, I’d walked upstairs and opened the door to our bedroom and my wife bolted up and knew something was up. I put the call on speaker and she heard everything after the high risk triggers.
“All tests have come back negative for anything, but there is a 7-10 day window that we can’t have test results for. [some more conversation about that] When there is a donor who is not labeled as high risk, they do not get this testing and scrutiny.”
“Are you able to tell me the age of the donor?”
“Yes, let me look that up… he is between the ages of, I can give you a 10-year band, 19 and 29 years old.” So there we had two pieces of information: age and gender… and we could already assume size because too much a size difference will automatically exclude my name from printing. She couldn’t tell me any more because the donor system doesn’t want you matching information up with accident reports, which would negate privacy if the donor family wants that.
We discussed the high risk portion back and forth for a couple of minutes and she volunteered to call me back in 10-15 minutes. You are allowed to turn down an offer for high risk lungs, but you can’t for “normal” lungs. We both said our pros and cons about accepting this offer. Quietly, to myself, I didn’t want to spend too much time on the topic because the statistics are that there is an actual 50% chance that donor lungs will be turned down before transplant. Not a 50/50 chance by probability but 50% statistically.
In the end, we landed on the choice to accept on the grounds that these lungs have already passed all the tests that would exclude them and Dr. Patel (the head pulmonologist) paired me with these lungs because I was the right size, they were performing admirably, and they had passed all in-donor tests.
“We accept your offer of these lungs. Now what?”
“How long does it take you to get here?”
“It’s a 30-45 minute drive plus waiting for backup to arrive here for the kids… we can be there at 5:00 or 5:30.”
“5:00 would be better. Come to the ER. You already have a room reserved but registration is in the ER this early.” She later called back and said that main registration opens at 5:00, so go there instead.
 After my wife’s parents arrived to be here when the boys woke up, we went to tell our 7yo we were leaving to get Dad his new lungs and then we left. There was absolutely no traffic on the way since we left at 4:10 and I experienced the full range of emotions every 3 minutes. My life was about to change. Someone has lost their twenty-something son. I’m about to be torn apart and put back together. We made such good time, I called Shari back when we were about to cross the bridge to Davis Island to TGH and she said to go to the ER.
After my wife’s parents arrived to be here when the boys woke up, we went to tell our 7yo we were leaving to get Dad his new lungs and then we left. There was absolutely no traffic on the way since we left at 4:10 and I experienced the full range of emotions every 3 minutes. My life was about to change. Someone has lost their twenty-something son. I’m about to be torn apart and put back together. We made such good time, I called Shari back when we were about to cross the bridge to Davis Island to TGH and she said to go to the ER.
We parked in the garage and got the 3rd slot from the ground level slant on the way up from the “basement” entrance. The perks of being up before roosters even think about waking up Farmer John! We walked the nearly half-mile walk to the ER because I wanted to remember what these lungs feel like doing that walk for potentially the last time.
The hospital
In the ER
 In the ER entrance, I went to the security guard at what is normally the check-in desk. “I’m here for my lung transplant. Do I check in at this desk?”
In the ER entrance, I went to the security guard at what is normally the check-in desk. “I’m here for my lung transplant. Do I check in at this desk?”
“You’ll see that young lady over at that desk. Right on about your lung transplant!” I loved this guy immediately. A 50-60 year-old powering me on with a “right on!” is just plain cool at 4:50am… any day of the week.
We started check-in and he sauntered over and leaned on the column next to me and said, “My girlfriend had a lung transplant 16 years ago. [he waited for registration to say something for a second] She has cystic fibrosis.”
“No kidding! So do I! I’m 38 and ready now. Then we’ll run a 5K together to celebrate.”
“She was 38 when she had it done. Wow! Yeah, man, she ran the Gasparilla 5K a year to the day she had hers.” You see, CFers really do great with new lungs. I did the quick math in my head and that makes her a 54yo CFer. He wished me well and escorted us to a private consultation room to wait for transport. I later referred to it as our “cry room” because it felt like this is where they take you to give you bad news so you can cry privately. The second my wife went to the bathroom, transport arrived, so I sat in the wheelchair awkwardly for a while. “As long as that was the worst of the day, today is going to be great,” I thought.
In the room
I was transported up to a room just a few doors down from where I spent the better part of a week in January during my transplant evaluation and settled right in to await the flurry of tests and exams that we knew to expect.
Only nothing happened.
They took my vitals, did all of the normal admission intake questions, gave up on getting my pulse oximeter to work, and left. For the next couple of hours, they’d come in and say they were still waiting for the doctor’s orders to go into the computer. We started to suspect that something was going wrong with the donor.
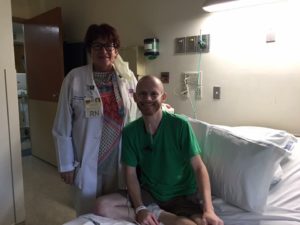 Eventually Shari arrived and gave me the high risk consent form and answered any remaining questions we had about that and about the process of timing between the donor site and TGH. Here’s what happens:
Eventually Shari arrived and gave me the high risk consent form and answered any remaining questions we had about that and about the process of timing between the donor site and TGH. Here’s what happens:
- The process started when this patient was brain dead and they were keeping all the organs going with a heart/lung machine, giving him medication, and doing all the things that would happen in a body if the brain was functioning.
- Every hour or so, they ramp up the ventilator to 100 and let the lungs soak up as much O2 as possible, and then take an arterial blood gas (ABG) test to see what the O2 and CO2 are doing. She described him as being “in the 500s” and they will often take lungs in the 300s. I asked if that means he is a “fit person.” “Yes, very fit.”
- The doctors there had already performed blood tests, a bronchoscopy, and other exams in order to offer the lungs with accurate information. This is how Dr. Patel and the surgeon decided to go forward with an offer to me.
- When I accepted the offer, they sent our team there, which includes one of the other surgeons to retrieve the lungs. What I didn’t know is what happens next.
- When all transplant teams are present, they start with the chest and open up the donor as if it’s a surgery and take a look at the lungs first, then the heart. That team steps back and another team looks at the liver, then one for the intestines, kidneys, and so on and so on.
- When everyone has made their initial inspections, they begin harvesting organs. Lungs are the most delicate and are viable for the shortest time. Once they clamp the blood supply to the lungs, they have 4 hours to get them sewn back into someone else.
As we continued to learn, we found out that the lungs were some distance away, not at all local. She left saying that our surgery time looked like noon. This was at about 6am. When she was wrapping up talking to us, people were lining up outside my door to do exams because the doctor’s orders were being received by various departments.
First, the cardiology tech sorta forced his way in because he had a full list to get to and he did my EKG. The mobile x-ray machine was out in the hall and got line-jumped. I thought that was pretty hilarious, because he waited patiently at least 5 minutes while we talked to Shari. He came in next as Shari left and said that Mitch would be replacing her at 7:00.
 Next, the vampire came in and drew all of these vials of blood plus another that is the verified tissue type test. For those not counting, that’s 17 vials of blood. No sweat.
Next, the vampire came in and drew all of these vials of blood plus another that is the verified tissue type test. For those not counting, that’s 17 vials of blood. No sweat.
Next, the RN tried to start an IV somewhere besides my elbow pipeline that I draw blood from. She failed. Twice. I wasn’t happy, but I was there to get new lungs, so I gave her a heap pile of grace and sent her on her way.
Next, her replacement RN started it with one try a couple of inches above my elbow in my biceps vein. No sweat. At this point, the most pain I experienced was my headache from coughing. It was throbbing pretty good, but I knew they wouldn’t give me any relieving opiates for it, so I didn’t even say anything.
With fluids going in at a staggering 15mL of normal saline (no glucose) per hour, they declared me all set when they found a pulse oximeter that worked… and then they left me alone.
A day of updates
At 7:20, Shari came back (after her shift ended) to tell me that the surgery time was being pushed back to 2:00 to accommodate another transplant team at the donor site. No sweat, I can wait another two hours.
Next, around 8:00, Mitch made his appearance and introductions. I signed the consent form and he informed us that the surgery time was now more like 4:00.
 Then it got really, really quiet. No updates. No nurses. Just us in a tiny private room waiting for word that our lives were forever to be different. My wife went down to the car to get food and eat it in the cafeteria where they have microwaves. I tried to sleep, but my heart was still doing 100+, as it had been doing for several hours. It was doing 120+ until Shari left and had filled us with calming information. Later in the day, I actually got it down into the 80s… and I was at 100% saturation on 5L/min ALL DAY. I was fit to be transplanted.
Then it got really, really quiet. No updates. No nurses. Just us in a tiny private room waiting for word that our lives were forever to be different. My wife went down to the car to get food and eat it in the cafeteria where they have microwaves. I tried to sleep, but my heart was still doing 100+, as it had been doing for several hours. It was doing 120+ until Shari left and had filled us with calming information. Later in the day, I actually got it down into the 80s… and I was at 100% saturation on 5L/min ALL DAY. I was fit to be transplanted.
The only people who kept showing up were the respiratory techs to give me albuterol and the floor techs who did vitals every hour or two. Housekeeping even came by twice!
Around noon and soon after, a couple of friends from church swung by to see me, encourage me, take part in our big day, and to pray for me. They both have several younger kids my oldest’s age and younger, so I felt better if they had masks on. It’s generally a good practice in the hospital anyway – I have worn a mask at TGH for years.
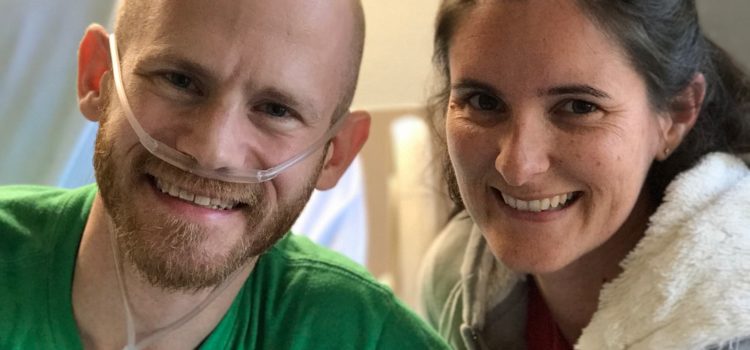
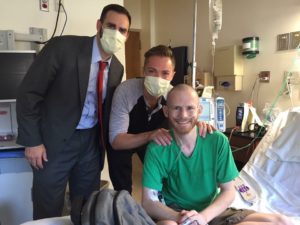 We got them caught up on the day so far and what was planned. Some time was spent geeking out with phone and phone cameras, so we got the nice photo in the post header out of it. It’s now my favorite photo of us… because it really was a fantastic day together. In the end, they really helped pass the time. I think it was about 1:20 when they left and it was quiet again. The original surgery time would have had me opened up and a lung coming out by that time, but we were looking at the 4:00 goal now.
We got them caught up on the day so far and what was planned. Some time was spent geeking out with phone and phone cameras, so we got the nice photo in the post header out of it. It’s now my favorite photo of us… because it really was a fantastic day together. In the end, they really helped pass the time. I think it was about 1:20 when they left and it was quiet again. The original surgery time would have had me opened up and a lung coming out by that time, but we were looking at the 4:00 goal now.
The Fellowship of the Lungs
Okay, that heading is ridiculous literary shenanigans, but soon after, my parents and my wife’s mom arrived to preside over passing time. By this point, though, I was getting pretty tired because I 1) got up at 2am, 2) hadn’t had anything to eat or drink since 3am, and 3) had been running on adrenaline for about 10 hours. I tried to sleep to pass the time and ignore my pounding headache.
“Meester Patterson, I’m here to give you your breathing treatment.”
sigh
 Now it was 2:00 and I decided to wait until 2:30 before I bothered Mitch for an update. Call him, I did. He said the OR at the other hospital was really busy and donor surgery was pushed back to 4:00, so we’d be looking at 6:00 or a bit later for surgery here. Another setback, but it was just an “I’m exhausted” thing because we knew this sort of thing happens almost every transplant. Sometimes people wait 19 hours or more. I was prepared and ready to keep my spirits high as long as I didn’t hear any indicators of uncertainty or bad news.
Now it was 2:00 and I decided to wait until 2:30 before I bothered Mitch for an update. Call him, I did. He said the OR at the other hospital was really busy and donor surgery was pushed back to 4:00, so we’d be looking at 6:00 or a bit later for surgery here. Another setback, but it was just an “I’m exhausted” thing because we knew this sort of thing happens almost every transplant. Sometimes people wait 19 hours or more. I was prepared and ready to keep my spirits high as long as I didn’t hear any indicators of uncertainty or bad news.
More trying to rest and pass the time. What I really wanted to do was unhook from my IV and pace the halls.
I was watching that clock and seeing the first number keep changing. I’d been done with all of my tests since 8am and the day was finally starting to drag on when 4:00 rolled around and no one had come to get me. In fact, I was still in my street clothes. At 4:20, my nurse came in and said they plan on coming in between 5:00 and 5:30 to take me down to pre-op. Before that, she was going to bring in some warm sanitizing cloths to give myself the modern version of a sponge bath and change into my XXXXXXL hospital gown.
5:00 came and went.
Then 5:30 came and went.
At 6:00, my nurse reported that Mitch was standing at the nurses station literally staring at his phone and waiting for a call from the surgical team. So at this point, all is good and we are still a go for launch, but we need to hear from them to get ready for perfect timing. I was like a cobra ready to strike, ready to jump into action at the hint of a moment’s notice.
At 6:15, the second in command pulmonologist walked in. I wasn’t at all alarmed by her straight face but I was suddenly on alert to see her instead of the nurses.
“So, when they got the lungs out of the donor, they just didn’t like how they looked, so they made the decision to not give you these lungs. They just weren’t good. I ordered you a tray and we’ll get you some food and get you discharged. It’s very quick without any extra paperwork.”
My thought wasn’t “After all this time!?!” but rather, “But everything was so perfect right up until getting them out of the donor?!?”
My nurse brought me a deli turkey sandwich, juice, applesauce, and 2 Pepsis. I scarfed like I hadn’t seen food in a week and then I was ready to go home. So we did.
Being okay with disappointment
As we performed an autopsy of the day in the car on the way home, neither of us felt bad. Exhausted but not bad. Disappointment really isn’t even the right word because there was also so much relief built into this answer. I didn’t have a hugely painful surgery that day and she didn’t have to stay up half the night and rush back the next morning.
Now it’s time to write about the emotions and processing the dry run.
As I sit here writing this after numerous sessions today because of the boys, I think I should draw this to a close at 3,100 words… (and now the next morning because I fell so hard asleep creating the box below). Here is the TL;DR for busy people:
Too long, didn’t read
I got THE CALL at 2am for a perfect match from lungs in a far away state and rushed to get all of my tests done for transplant by 8am. After several delays to the surgery time, they sent me home at 6:30pm because the surgeon didn’t accept the lungs once they were out of the donor – they were bad.
Wow – thanks for walking us through your day….may the real “day” come soon! Praying it does!
We’ve seen countless times in the transplant stories and Facebook transplant groups that it almost always happens within 2 weeks of a dry run. Time to rest up! 🙂
I too missed a pair, I missed mine due Fl declaring “State of Emergency” for hurricane. All small aircraft grounded. Very unfortunate for me but the lungs went to a recipient within driving window of his surgeons, it Was his “Right Lungs at Right Time?”♻️.
Dr. Patel and his associates , turned down 2 other offers for one reason or another.
I finally received my gift at the right day and time, just 3 days befor ECMO. 12/12/16. I’m forever grateful to my support team aka my wife, the Dr’s and their staff’s and last but not at all least my Donor and his family?♻️??
I don’t regret the day at all. It was actually one of my best days in a looooong time. Felt so alive. So much love. So close to my wife. I wouldn’t trade my dry run for a transplant without one now. Not for “knowing what was going to happen” like so many (because we already knew all of this was expected) but rather because of the privilege of experiencing life to its fullest.
Jesse, praying for you. We’ve seen a lot of miracle work through the Lord Jesus and our church so I will be bringing this up to several of our prayer warriors. God is on your side, these things happens in order for us to have a way to glorify Him. I pray you get your lungs this week! I’ll be looking for your updates. Thank you for sharing this incredible adventure and great writing! When’s your book coming out!?
Thanks, Paul.
Funny you should mention a book… yes, I have one planned and it will be no problem after laying down all of these words. I’ll probably write and edit it through 6 months post-transplant and do it right so it will be available on Amazon and add a secure shop to this site to live on as an information mother lode for everyone awaiting a transplant for themselves or a loved one.